Tendinopathies and Bursitis: An overview of causes and treatment.
Posted on 21st March 2023 at 15:35
By Carl Green
In this seventh post within my “types of musculoskeletal conditions series,” I will be covering the structure, function, and problems associated with tendons and bursa, and how you can improve the health of these areas. If you are interested in learning more about other types of musculoskeletal conditions, please take a look at my other posts in this series.
Tendon and Bursa Structure and Function
Tendons are found at both ends of our muscles and join/merge into the contractile muscle tissue at the musculotendinous junction. Tendons are made from connective tissue (mainly collagen) to act like stiff springs that store and release energy built up from the forces produced when moving our bodies, particularly decelerating us against gravity. They also have an essential role in attaching our muscles to the skeleton/bones, and without them the muscle would not have the strong and adaptable anchor points needed.
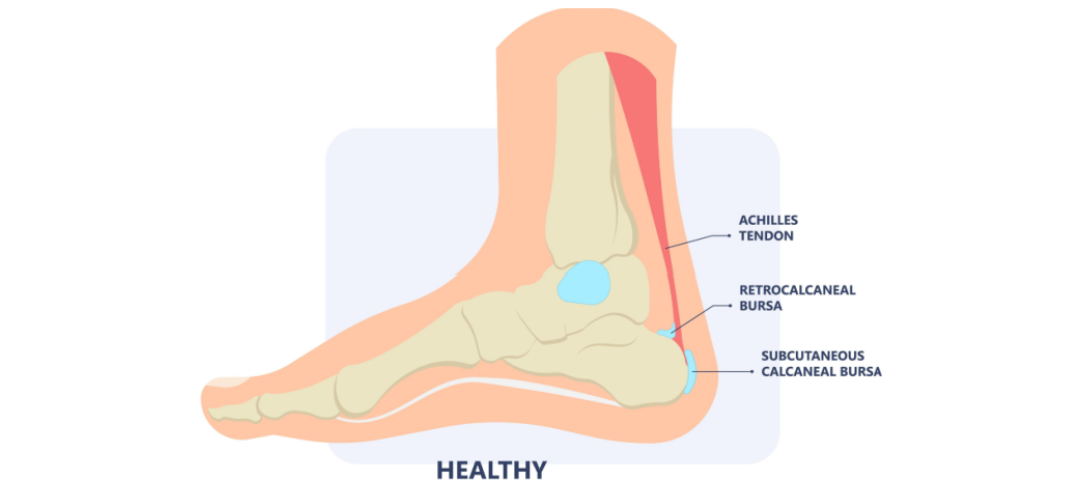
Bursa are integral fluid-filled sacs found between soft tissues and bones all over the body. The size of these vary from millimetres to several inches, and they tend to be fairly flat. Their main function is to reduce friction and compression, as a form of protection for our musculoskeletal tissues.
Tendinopathies
The term tendinopathy refers to problems associated with tendons. These can be categorised in a number of ways, but one of the more up to date and straightforward is the continuum model. This includes reactive (stage 1), disrepair (stage 2), and degenerative (stage 3) tendinopathies.
Reactive tendinopathies usually involve days to weeks of tendon hypersensitivity and swelling in response to a recent significant increase in workload, particularly when the tendon is also in a compressed state. An example of this could be doing spring cleaning, or significant work in the garden, that is not typical of most weeks or months, or taking up running for the first time and building up too fast or possibly with muscle weaknesses and altered movement/biomechanics. These relatively short term increases in activity can cause an overload to the tissues leading to symptoms.
Tendon disrepair is where a reactive tendinopathy becomes frequently flared up over weeks to months, and the stresses cause a persistent cycle of “micro-damage and repair”. The circulatory and nervous systems change within the tendon, increasing sensitivity, leading to the tendon becoming less efficient at tolerating and withstanding physical stresses/forces. If the condition is not managed effectively, or isn’t responding to mainstay treatments, the tendon can become unable to fully repair effectively, leading to a degenerative tendinopathy.
Degenerative tendinopathies are associated with permanent changes to tissue structure. This often includes irregular thickening as well as a reduction in tendon cells, leading to weakness and reduced tendon stress tolerance, and healing potential. This is the stage of tendinopathy we want to certainly avoid, and this is why timely treatment (within the first couple of months) is important.
Bursitis
This term is translated to “bursa inflammation” and a pocket/balloon of soft contained swelling is the main symptom, sometimes with associated pain. The most common locations are prepatellar bursitis (kneecap), olecranon bursitis (point of elbow), retrocalcaneal bursitis (Achilles heel), subacromial bursitis (shoulder), trochanteric bursitis (outer hip), and popliteal bursitis or cyst (back of the knee, also known as a bakers cyst).
Bursa can become inflamed due to traumatic injuries, infections, or compressive stress, such as frequent direct pressure or moving the body in a way that excessively pulls the bursa and often neighbouring tendons hard against underlying bones.
Treatment of Tendinopathies and Bursitis
Tendinopathy's and bursitis share similar risk factors that increase the likelihood of causing problems. These include obesity, hormonal changes, steroid and antibiotic use, and poor fitness (strength, mobility, cardiovascular health, coordination and movement).
As explained previously both conditions are also flared up from overloading which is often linked to our behaviour, habits, and general health. Therefore to fully address the problem, it is often essential with both of these conditions to fully understand what contributing factors exist in your individual situation, and to provide education and advice to change your behaviours to reduce their impact. Treatments include specifically tailored pacing, or load management guidance to reduce excessive tissue stress and working around the limitations. This allows the body an opportunity to settle, and can prevent a temporary reactive issue from becoming more problematic and potentially permanent.
Another important aspect is strengthening to improve soft tissue (particularly tendons in this case) capabilities, and potentially improve biomechanics to reduce tissue stress. Therefore, conditioning your body to improve its tolerance to mechanical stress and the demands of your individual lifestyle. Loaded/weighted strengthening exercises should be tailored to your lifestyle, tissue capacity, and progressed at the right time. This is not only a mainstay treatment for these problems, but can also potentially help reduce the likelihood of recurrence.
In regards to symptoms and flare up relief, this can be aided in many ways including taping, use of supports and straps, medication, ice and heat, gentle exercise/movement, and manual therapy (various massage, mobilisation and manipulation techniques). Also shockwave, acupuncture, and ultrasound all have limited evidence to support their use, and can be worth considering, but should not be relied on as primary treatments, or used in isolation.
Other non-physio treatments such as injections (for example corticosteroid) or aspirations (draining) are sometimes considered, but are often unnecessary in many cases.
What's next?
If you have any questions about tendinopathies and bursitis, any other topics within the musculoskeletal series, or are interested in our support, please get in touch with us at Colchester Physiotherapy and Sports Injuries Clinic. Myself (Carl Green) or my physiotherapist colleagues Craig Fowlie or Jane Marr will do all we can to help you.
The next instalment in this musculoskeletal conditions series will be on osteoarthritis and stenosis, so check back in for that, or follow us on social media to see when it is published.
Get in touch with the team here at Colchester Physiotherapy and Sports Injury Clinic for honest advice and recommendations!
Other Articles in our Musculoskeletal Condition Series
Author
Carl Green

Carl is a Specialist Musculoskeletal Physiotherapist, Sports Science and Human Biology graduate, former Lecturer in Sport and Exercise, Personal Trainer, and Sports Massage Therapist.
He has worked as a Physio within the NHS at a senior level, sports injury clinics, his own practice, stroke rehabilitation, occupational health and chronic pain. Carl also has first hand experience of acute and chronic injuries, pain, surgery, and disability, giving him a deeper understanding how these can affect us both physically and psychologically.
He started his career in health and fitness in 2002. Empowering people to achieve their goals, overcome challenges, and reduce future problems through lifestyle/behaviour change and exercise has continued to be a big part of his approach as a Physio.
Carl has tried many sports, but mainly focused on rugby, gym training, running (5k to half marathon), and Muay Thai Boxing. He also enjoys snowboarding, home gym training, teaching his dog tricks and playing fetch, covering songs on his guitar, and has recently taken up archery.
Tagged as: Musculoskeletal Condition Series
Share this post: